Exercise Recommendations
The American Diabetes Association recommends that a person with diabetes aims for 30 minutes of moderate-to-vigorous intensity aerobic exercise at least 5 days a week.
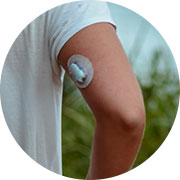
Medicare CGM
Medicare covers therapeutic continuous glucose monitors (CGMs) for people with Type 1 & 2 diabetes and using insulin.

Glucose Recommendation
The American Diabetes Association suggests (postprandial) glucose of less than 180mg/dl.
Ketosis means that there are larger-than-normal amounts of ketones in the bloodstream.
There are a few different kinds of ketosis, but for people with diabetes there are two major ones:
Dietary ketosis: When we don't eat enough carbohydrate to fuel our bodies, we start using fat for energy. This is the basis of "ketogenic" diets. The byproduct of the breakdown of fats for energy is a fatty acid called a ketone. Dietary ketosis generates small to moderate ketones that go away quickly when we start eating carbohydrates.
DKA: The second, and more dangerous type of ketosis for people on insulin is Diabetic Ketoacidosis, or DKA.
When our bodies do not have enough insulin to be able to use carbohydrates for energy, our body starts using fat for fuel and producing large amounts of ketones as byproducts. Because high blood sugar also tends to occur when the body does not have enough insulin, dehydration also occurs. The combination of ketones and dehydration can make our blood very acidic. When our blood is acidic we get very sick: nausea, low energy, slurred speech, clouded thinking, deep/labored breathing, heart rate changes, eventually loss of consciousness, and organ failure that can be fatal.
Unlike dietary ketosis, only taking insulin will reverse DKA. Additional treatment includes hydration and electrolyte balancing with IV fluids.
People on long acting insulin are at risk for DKA when doses are reduced dramatically or forgotten. People on pump therapy are at risk when they experience a tubing or site occlusion or extended disconnection. People taking oral medications for their diabetes are at rise of DKA if their pancreas loses the ability to sufficiently produce insulin and blood sugars become very high.
Monitoring for ketones (using urine test strips or blood meters that measure ketones) anytime we have an unexplained high blood sugar can help prevent DKA. When ill, it is important to continue taking one’s insulin, stay well-hydrated, and monitor ketones. Persons using insulin should work closely with their physician and a registered dietitian before attempting a ketogenic diet plan.
Glycosylated Hemoglobin A1C (HbA1C), often called A1C testing, is a measurement of the average blood glucose level over a roughly three-month period. Red blood cells carry oxygen and nutrients around our bodies. Oxygen hitches a ride on red blood cells by attaching to hemoglobin molecules. But glucose present in our blood stream also sticks to hemoglobin on the red blood cells. Just like spilling pancake syrup makes everything we touch more sticky, having excess glucose in our bloodstream means that more and more of those hemoglobin molecules get coated in glucose. This process is called glycosylation. The A1C is measuring the percentage of red blood cells are glycosylated.
Since red blood cells tend to last for about three months, A1C is a measure of the average blood sugar those cells have been exposed to over the most recent three-month period. Most people with diabetes should have an A1C measured every three months. Those with type-2 diabetes often have theirs checked every three or six months. A1C tests are measured by a blood sample, either from an IV blood draw in a lab (the most accurate method) or from a finger stick blood sample in a medical office where available. There is no need to fast for an A1C test and time of day does not affect the result. Be aware though that certain blood disorders such as anemia can cause the A1C result to be inaccurate.
The A1c is important because a high A1C has been shown to increase the risk for long-term diabetic complications such as eye disease, kidney disease, nerve disorders, heart attack and stroke. The American Diabetes Association recommends that most adults with diabetes keep their A1C below 7%.
Whether you have 20/20 vision or have worn glasses since grade school, an annual eye exam is critical for anyone with diabetes… no matter your level of blood sugar control.
Diabetes-related retinopathy is the leading cause of blindness in adults ages 18-65 in the United States. Retinopathy is caused by the over growth and leaking of blood vessels behind the retina of the eye. Think of the eye like a movie theatre: there is the camera with its lens sending a focused image. That's your corneal lens. Then the image is visible when it shines on the screen. That's your retina. Now imagine what would happen to that picture of we painted a bunch if lines across the screen (blood vessel over growth) or splashed buckets of black paint across it (blood vessel leaks/bleeds). We can no longer see the picture, and undoing the damage is typically impossible. However we can do a LOT to prevent vessel growth and leakage! But the first step is to know there is a problem BEFORE vision is lost.
An annual dilated eye exam by an optometrist or ophthalmologist is ideal. There is no prep required for this exam. The doctor will administer a drop of numbing fluid and a drop of dilating fluid in each eye. They will inspect the retina carefully, and may take a photograph. This is a painless exam and most people are able to return to normal activity within a couple of hours. Because the eyes remain dilated for several hours, some may want to wear sunglasses for the rest of the day.
We often say that the eyes are the window to the soul. Well, they are certainly the window to your bodies! Annual eye exams can catch early signs of diabetes, glaucoma, hypertension, cancer, neurologic injury, high cholesterol, rheumatoid arthritis, stroke risk, lupus, thyroid disease, aneurysm and more! An annual eye exam can save your vision, and even your life!
For more information on dilated eye exams and the importance of annual eye exams, visit https://nei.nih.gov/learn-about-eye-health/healthy-vision/get-dilated-eye-exam.
It is estimated that 30% of people with diabetes will experience a non-healing foot wound or ulceration in their lifetime. More than 80% of lower limb amputations in the US start with a foot ulcer. These statistics are scary, but there is a silver lining. Foot examinations reduce amputation risk by 85%!
The most common complication of diabetes is peripheral neuropathy, nerve damage that reduces sensation at our extremities, most commonly our feet. This increases the likelihood that a wound can develop without being noticed. Our second most common complication is blood vessel disease. Reduced blood flow leaves us more susceptible to developing wounds and slows wound healing. Elevated glucose levels can also “feed” fungal and bacterial infections.
The first and best prevention is good blood sugar control. Managing blood sugar levels reduces glucose available to feed infections. It also reduces inflammation, thickening, and stiffening of blood vessels that reduce blood flow.
Self foot care for people with diabetes should always include:
- Looking at your feet daily; watch for changes in color, changes in texture, warm temperature, calluses, and cuts. You may need the help of a mirror to see all sides of your foot.
- Washing feet daily using moderate-temperature water and making sure to dry thoroughly.
- Maintaining blood flow to the feet is very important.
- 30 minutes per day of moderate physical activity.
- Avoiding restrictive clothing such as tight socks or stockings.
- Avoid positions that apply pressure such as prolonged sitting, crossing legs, or remaining in one position for a prolonged time.
- Making sure that shoes do not press or rub. Most people with diabetes can obtain a pair of specialty shoes covered by insurance each year.
- Trimming nails straight across and filing the corners to reduce the risk of ingrown nails.
- Avoiding shaving, scraping or removing one’s own callouses.
- Preventing over drying by using an unscented moisturizer on the foot everywhere but between the toes.
If you notice a change or issue with your feet, seek medical assistance immediately. Putting off treatment could make the problem much more difficult to treat. In most cases, people with diabetes are covered for podiatry or nursing services to perform foot care that cannot be provided independently.
Life with diabetes is filled with ups and downs. We are often under-educated that medications bring our blood sugars down and sugar makes it go up, and that’s it. But it is SO much more than that! In fact, there are so many factors that affect blood sugar that it is virtually impossible to achieve “normal” blood sugar control all the time. Even people without diabetes experience out-of-range blood sugars sometimes.
STUFF THAT LOWERS BLOOD SUGAR:
Blood sugars are typically lowered by insulin and by muscle uptake of glucose – especially when we are physically active. There are many diabetes medications other than insulin that help to lower blood sugar – some by stimulating more insulin production, some by reducing the body’s production of its own sugar, some by improving our cells’ sensitivity to insulin, and some by blocking the digestion of carbohydrates. We also lose some sugar to urination whenever blood sugars are above 180 mg/dl, and there are medications that can make this happen even at lower levels. Mental stimulation can also lower blood sugars since our brains burn glucose for fuel. There are some non-diabetes medications that can cause blood sugars to drop, so always make sure your entire healthcare team knows about all of the medications you are taking.
STUFF THAT RAISES BLOOD SUGAR:
Foods raise blood sugars, particularly carbohydrates. But our bodies also convert proteins into blood sugar. Sudden stress can elevate blood sugars very quickly, while chronic stress can raise blood sugars moderately over long periods of time. Stimulants like caffeine, steroid medications, nasal decongestants, and ADHD medications can also raise blood sugars. If you are starting on these medications be sure to ask your prescriber for a plan for blood sugar monitoring and management. Illness often pushes blood sugars up, particularly severe infections or fevers, Insulin resistance (the body’s cells’ inability to use insulin properly) also raises blood sugar. Things that increase insulin resistance include physical inactivity, weight gain, and high fat meals (which cause temporary insulin resistance). Managing weight, maintaining routine physical activity and reducing high fat food intake help reduce this impact.
Glucagon is another hormone that can raise blood sugar, by stimulating the liver to secrete sugar into the bloodstream. Our bodies make glucagon in response to low blood sugar, unless too much insulin is present (glucagon production is blocked by insulin). However, glucagon can be administered via injection as a rescue for severe hypoglycemia.
Life with diabetes has its share of struggles. For one thing, it can become pretty expensive. However, there are a few health insurance perks that many people are not aware of. Here is a rundown of services that are covered by private insurance a well as Medicare and most, if not all Medicaid MCOs.
Dietitian services: Just about everyone with diabetes is covered to see a registered dietitian for "Medical Nutrition Education." This can include information on carb counting, weight loss, menu planning, and other diabetes related topics (Tip: if you also have hypertension, or other cardiac diagnoses, you can also get additional hours of dietary education related to that as well!)
Diabetes education: Newly diagnosed individuals are typically approved for at least 10 hours of diabetes self- management education in their first year after diagnosis and additional hours of education every year thereafter. This includes education on how to better manage your diabetes, updates on the latest medications and technologies, tips on how to eat right and exercise safely, stress management, glucose monitoring techniques, and much more.
Shoes: Most people with diabetes have coverage for a pair of approved shoes per year. Modern, attractive styles are available from durable medical supply companies and online suppliers.
Podiatry: People with diabetes are entitled to coverage for foot care services including nail trims, exams, callous debridement, and even orthotics!
Vision exams: Even without "Vision coverage" plans, people with diabetes are entitled to an annual dilated eye exam covered as a medical benefit.
Workout and diet services: Many insurance plans offer discounts and reimbursements on gym memberships, meal delivery services for weight management, even sneakers!
Tech: Most insurance carriers cover Continuous Glucose Monitoring for patients on insulin, and many are even beginning to cover them for patients taking oral medications (particularly if you've had a hospital stay for a diabetes-related complication). More and more insurance companies are also partnering with technology companies to provide their customers with apps and other digital management technologies free of charge.
Case management: Most insurance companies now provide people with diabetes a Care Manager. This is typically an RN or Social worker trained in helping you pull all the pieces together and navigate the healthcare system. This person can advocate for your needs, communicate with providers, and help you stay on track with meeting your management goals.
One of the best ways to manage and prevent diabetes is through physical activity. The American Diabetes Association recommends 150 minutes of physical activity weekly (including two or three days of resistance/strength-training exercise). This is important not only for improving blood sugar control, but also for reducing the risk of heart disease. But there are more benefits! Exercising 30 minutes daily increases insulin sensitivity. This can lead to a reduced need for medication or insulin, and even prevent/postpone the onset of diabetes for those with prediabetes. The effects of exercise last for just a day or two, so making physical activity a regular and routine part of your life is key.
Physical activity is also key to weight control as it helps us burn calories, build lean muscle and increase metabolism. Daily physical activity can also provide mental health benefits and stress relief
Another great benefit of physical activity is that it can help lower blood sugars pretty quickly. When we have blood sugars that are higher than desired (such as after meals), we can use physical activity to bring blood sugars back to our target range. For example, taking a walk after dinner.
Getting daily physical activity does not mean you have to sign up for a gym membership. From playing with the grandkids, gardening and walking with friends (human or animal!) there are endless sources of physical activity. The important part is to maintain duration, intensity and frequency. Moderate level physical activity is when our heart rate and breathing pace are elevated, but we are still able to speak with minimal difficulty.
For those on medications that can lower blood sugar such as insulin and sulfonylureas, work with your prescriber to develop a plan to avoid hypoglycemia. Always have fast acting carbohydrates available to treat low blood sugar should it occur.
What are realistic goals for diabetes management? It is important to remember that individual blood sugar target ranges should be established with your prescriber, and individual medical risks, lifestyle needs and other risk factors can vary.
The American Diabetes Association recommends that adults keep their A1C below 7%, which corresponds with an average blood sugar below approximately 150 mg/dl. Those at risk of severe injury from hypoglycemia (such as young children) should aim for an A1C of 7.5 (average below 170 mg/dl). However A1C is just an average of the last 3 months. Someone with frequent low blood sugars might have a low A1C, but this does not represent quality diabetes management.
Besides A1C, it is often recommended to keep one’s blood sugar within a healthy range as often as possible. For example, your healthcare provider might recommend a target of being between 70 and 160 mg/dl at least 70% of the time. This gives approach addresses both the overall average and the stability of your blood sugar levels. Extreme swings from high to low and back again can be just as damaging to our wellness as a high overall average. Steady blood sugars are indicated by a number called standard deviation (SD), a measure of how much one’s blood sugars stray from the average. For most people, an SD below 50 demonstrates fairly steady control. People who do not have diabetes typically have an SD of about 20.
Another important target for people with diabetes is blood pressure. Everyone should shoot for a blood pressure below 120/80. People with diabetes should consider treatment to reduce hypertension with a blood pressure of 140/90 or higher.
Targets are an important part of management, but it is important to remember that we are far more than numbers! Who we are: our life goals, our mental health and personal needs are all just as important as reaching target numbers.
One of the most common questions about diabetes has to do with overnight blood sugars. "Why is my blood sugar fine when I go to bed, but high in the morning? I’m not eating a thing after bedtime!"
There are a few things that can be at work here.
The first step in figuring out what caused an overnight blood sugar rise is to make sure the blood sugar returns to normal after an evening meal. Checking blood sugar 3 hours after your evening meal will give a good indication of this. When blood sugars normalize after your evening meal but then rise through the night there are two likely causes:
Dawn phenomenon: This is when the liver produces extra glucose in the early morning hours. This is caused by the body's hormonal and circadian cycles. Increasing physical activity through your week with at least 30 minutes of moderate physical activity daily can help reduce this by making your body more insulin sensitive. We can also use medication to curb overnight blood sugar rises. Metformin reduces the amount of glucose that the liver produces, and long-acting (basal) insulin can be added or increased to maintain steady blood sugars overnight.
Somogyi effect: This is when the liver releases glucose in response to a drop in blood sugar. Let’s say your blood sugar drops a bit too low in the middle on the night – not enough to wake you, but enough to cause your body to react by producing some stress hormones. Those hormones cause the liver to dump sugar into the bloodstream, resulting in a high reading by morning. If you have identified this pattern (by wearing a CGM or checking your blood sugar during the night), you can prevent it by having a slowly-digesting snack at bedtime or talking to your physician about reducing the insulin or medications you use at night.
Sugars are easy to spot on food packages labeling, they have names ending with -ose. Sucrose, dextrose, glucose, fructose, maltose and lactose are some examples. Ingredients ending in -dextrin or -extract are also a form of sugar. These include maltodextrin, dextrin, wheat dextrin and malt extract.
But sugars aren't the only sweeteners that affect blood sugar. Also look for juices and extracts. These include high fructose corn syrup, corn syrup, honey, agave syrup, maple syrup, caramel syrup and coconut blossom sugar. Just because a product says "no sugar added" doesn’t mean it is not loaded with other sweeteners that raise blood sugars!
Another type of sugar is sugar alcohols, which end in -ol. These include xylitol, erythritol, sorbitol and maltitol. These are found in most "Sugar Free" products. Sugar alcohols digest more slowly than ordinary sugars, and don’t raise the blood sugar quite as much. When carb counting, you can assume that half of the sugar alcohols will impact your blood glucose. One other note: When consumed in large quantities, sugar alcohols can cause gas, stomach cramps and diarrhea.
Some artificial sweeteners don't have any impact on blood sugar levels. These include: Cyclamate, saccharin, sucralose, aspartame and acesulfame K. These are typically found in "Diet" or "Zero calorie" products. However, many studies have shown that using these artificial sweeteners to replace sugars does not correlate to weight loss and may cause headaches or stomach upset.
Stevia and monk fruit are natural sweeteners without calories or sugar. They are obtained from plants and dried/powdered or turned into a liquid. These products are not always appropriate for baking, and may not dissolve well in drinks, so check labels for usage and how to swap them out in recipes.
Explore our Diabetes Product Catalog
Along with our product offering, our catalog offers valuable information about insurance coverage for diabetes supplies, education and more.
Visit Our Online Diabetes Catalog Byram Healthcare Diabetes Catalog